Understanding Fatigue: A Comprehensive Overview
Fatigue affects millions worldwide and is marked by persistent tiredness that rest does not relieve. Unlike ordinary tiredness, it can severely impact daily functioning, from work performance to social interaction and overall well-being. Often misunderstood as a result of stress or poor sleep, fatigue can signal deeper physical or mental health issues requiring thorough evaluation.
Its complexity lies in its dual impact on body and mind. Physical causes may include chronic illness, nutritional deficits, or respiratory issues, while mental fatigue often stems from anxiety or depression. These elements often interact, creating a cycle of physical and mental exhaustion. This highlights the need for a holistic approach to diagnosis and treatment.
Recent advances in medical imaging have deepened our understanding of fatigue, revealing how various physiological and neurological systems contribute to it. These insights help shift the perception of fatigue from a sign of weakness to a valid medical concern worthy of serious attention.
The Importance Of Lung Function In Energy Levels
Lung function plays a vital role in energy levels by ensuring that the body—and especially the brain—receives adequate oxygen. When compromised, as in conditions like COPD, asthma, or sleep apnea, poor oxygen delivery can lead to significant fatigue. Medical research confirms that reduced lung function lowers physical endurance and increases breathlessness, contributing to a cycle of inactivity and worsening fatigue. The body naturally conserves energy in response to low oxygen, leading to both physical and mental exhaustion.
According to the Workwell Foundation (https://workwellfoundation.org/), lifestyle changes are crucial for managing chronic fatigue. Their research highlights the importance of pacing, energy conservation, and the use of objective assessments such as Cardiopulmonary Exercise Testing (CPET) to guide safe activity levels in individuals with chronic fatigue-related conditions. Improving lung health through pulmonary rehabilitation, breathing exercises, and treatments like supplemental oxygen can significantly reduce fatigue. This underscores the importance of integrating respiratory and neurological care in managing chronic fatigue and improving overall well-being.
The Role Of The Brain In Fatigue
The brain plays a key role in fatigue, regulating energy and processing signals from the body. Neurotransmitters influence alertness, and imbalances can trigger fatigue even when the body is physically rested.
Beyond chemical signaling, structural and functional brain changes—seen in conditions like multiple sclerosis, chronic fatigue syndrome, and sleep disorders—also contribute to fatigue. Imaging studies reveal abnormalities in brain regions tied to energy regulation and cognition, underscoring the neurological basis of fatigue.
The brain’s response to fatigue is interconnected with other systems, such as the lungs and heart. Poor oxygenation, for example, can impair brain function and lead to cognitive fatigue. Understanding these links enables more comprehensive treatments that target both physical and mental contributors. Advances in brain imaging are helping researchers identify neural patterns linked to fatigue, opening the door to more precise, root-cause-focused interventions.
Lung Imaging: Understanding Respiratory Contributions To Fatigue
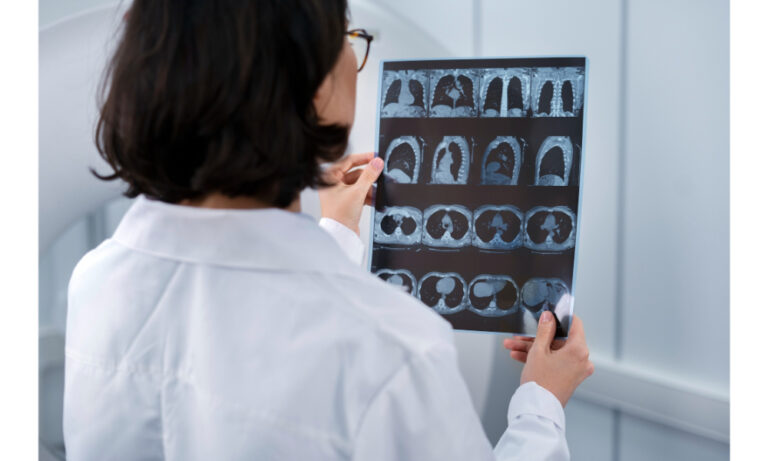
Lung imaging plays a key role in understanding how respiratory health influences fatigue. Techniques like chest X-rays, CT scans, and pulmonary function tests provide detailed views of lung structure and performance, helping identify conditions that may contribute to low energy levels. This information supports the development of targeted treatment plans that address both respiratory and neurological factors involved in fatigue. When signs point to overlapping cardiovascular concerns, a cardiologist’s perspective can offer additional insights, given the close relationship between heart and lung function in maintaining energy and endurance.
Imaging studies have shown that conditions such as COPD, asthma, and interstitial lung disease can impair lung capacity and gas exchange, leading to reduced oxygen delivery and increased fatigue. These findings underscore the need to consider lung health when managing persistent tiredness and limited physical endurance.
Lung imaging also helps track treatment effectiveness. Follow-up scans can evaluate improvements in lung function after interventions like pulmonary rehab, bronchodilators, or supplemental oxygen. This enables clinicians to tailor care plans that enhance both respiratory function and overall energy, improving quality of life for those affected by chronic fatigue.
How Imaging Techniques Illuminate Fatigue Causes
Advanced imaging techniques have significantly deepened our understanding of fatigue by uncovering the physiological and neurological mechanisms behind it. Tools like MRI, PET, and fMRI provide detailed, non-invasive views of the brain and body, helping identify structural and functional changes that may cause fatigue. These insights support more accurate diagnoses and targeted treatments.
Brain imaging has shown that people with conditions like chronic fatigue syndrome often exhibit reduced activity and altered connectivity in areas responsible for energy regulation, attention, and executive function. Such findings suggest that fatigue may stem from disrupted neural pathways, opening the door for brain-based therapeutic approaches.
Similarly, lung imaging techniques such as CT scans and spirometry help detect respiratory issues like airway obstruction or inflammation that can lead to fatigue. Identifying these problems is essential for addressing both neurological and respiratory contributors to fatigue. This integrated approach allows for more effective management strategies and improved patient outcomes.
Brain Imaging: What It Reveals About Fatigue
Brain imaging has become a vital tool in understanding fatigue, offering insight into the neural mechanisms driving this complex condition. Functional MRI (fMRI), for instance, allows researchers to observe real-time brain activity and has been key in identifying patterns linked to fatigue.
Studies show that individuals with fatigue-related conditions often exhibit reduced connectivity in brain networks responsible for attention, memory, and emotion regulation. These disruptions suggest fatigue may stem from the brain’s impaired ability to process and integrate information, highlighting neural pathways as potential targets for treatment.
In addition to functional changes, imaging has revealed structural differences, such as reduced gray matter volume in people with chronic fatigue syndrome. These abnormalities may explain the cognitive and emotional symptoms commonly associated with fatigue. Understanding both functional and structural brain changes is crucial for developing targeted interventions that address the underlying causes of fatigue.
Treatment Options Based On Imaging Results
Advanced neurological scans alongside complementary imaging techniques provide crucial insights that help uncover the neurological and respiratory causes of fatigue. This detailed understanding enables healthcare providers to develop personalized treatment plans that more effectively enhance patient outcomes and quality of life. For fatigue related to brain function, therapies may include cognitive rehabilitation to strengthen neural connections and improve mental clarity. Medications that balance neurotransmitters, such as antidepressants or stimulants, can also be used to address fatigue caused by chemical imbalances. When respiratory problems play a role, treatment often involves pulmonary rehabilitation through breathing exercises, physical therapy, and patient education. Medications like bronchodilators or corticosteroids may reduce inflammation and improve lung function. By addressing both brain and lung health, clinicians can adopt a holistic approach to managing fatigue and restoring energy.
Conclusion: Integrating Imaging Insights For Better Fatigue Management
In conclusion, advanced imaging techniques have deepened our understanding of fatigue by revealing the complex connections between brain and lung function. These tools have made it possible to identify structural and functional abnormalities, supporting more accurate diagnoses and personalized treatment strategies.
Recognizing fatigue as a legitimate physiological and neurological condition, not just a state of mind, is essential to improving care. Integrating imaging insights into clinical practice promotes a holistic approach that addresses both the mental and physical contributors to fatigue.
As imaging technology continues to advance, it will play an increasingly vital role in guiding effective, targeted treatments. This empowers healthcare providers to move beyond symptom management and helps patients regain energy, function, and quality of life.